Moesha Rudo Mavangira1, B. Optom Student
Tsering Lamu Shongmu2, Assistant Professor
1Parul University, Vadodara, India
2SGT University, Gurugram, India
Introduction
Posture refers to the position and alignment of the body in space. While often associated with musculoskeletal health, posture also plays a surprisingly critical role in ocular physiology. (1) Posture is commonly associated with spinal alignment and musculoskeletal health, which plays a surprisingly critical role in eye physiology. Specifically, posture can significantly affect Intraocular Pressure (IOP), the fluid pressure within the eye. A normal IOP ranges from 11 to 21 mmHg. Deviations from this range, especially prolonged elevation, are closely linked to ocular pathologies such as Glaucoma, Uveitis, and Retinal Detachment. (2) The regulation of IOP and thus ocular homeostasis is influenced by factors like aqueous humour dynamics, central corneal thickness, and notably, body posture. Among these, posture-related IOP changes are more prominent in eyes with existing Glaucoma. (3)
Head Position and IOP
Adopting a head-bowed posture, such as when reading, can considerably increase IOP. This happens mainly due to hydrostatic pressure effects, elevated Episcleral Venous Pressure (EVP), and choroidal vascular engorgement as fluid shifts towards the head. (3) While such posture-induced IOP changes occur in both healthy individuals and those with Glaucoma, the increase is significantly more pronounced in Glaucoma patients. (5)
Supine Position and Head Elevation
Lying flat in a supine position generally leads to higher IOP. However, this can be reduced by elevating the head with a thick pillow, which helps to lower IOP compared to lying completely flat. (5) This shows how the redistribution of gravitational fluid affects the eyes, especially when the vertical distance between the eyes and the heart reduces.
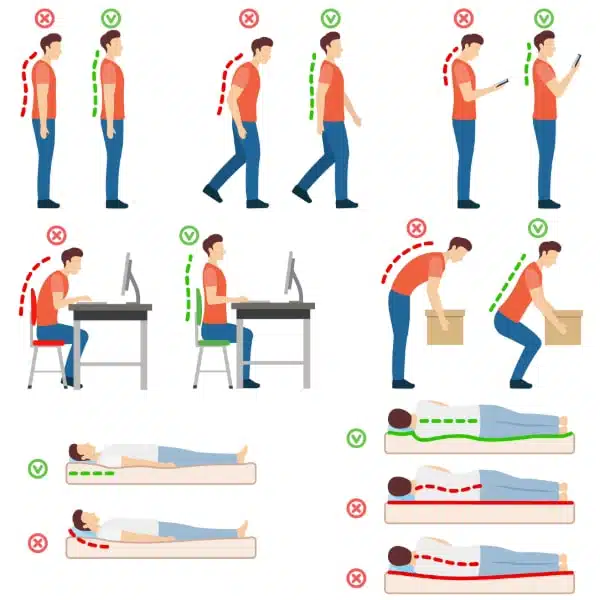
Figure 1: This image shows different body postures
Image Courtesy: https://fivedockosteochiro.com.au/2024/04/23/good-posture-get-the-best-tips-and-tricks/
The Autonomic Nervous System Role
The autonomic nervous system also plays a hand in regulating IOP. (6) For example, local administration of adrenaline can potentially reduce IOP by increasing the diameter of the Schlemm’s canal. Conversely, external factors like tight neckties can increase IOP by raising jugular venous pressure, leading to congestion in the choroid.
| Year of Study | Posture Type | Relative IOP Level | Physiological Explanation |
|---|---|---|---|
| 2023 | Sitting | Lowest | Standard reference position used in clinics. (8) |
| 2023 | Standing | Slightly high | Reduced episcleral venous pressure but postural adjustment. (9) |
| 2023 | Kneeling | High | Partial venous compression, reduced venous return. (9) |
| 2023 | Squatting | Higher | Increased intra-thoracic pressure (Valsalva effect). (9) |
| 2025 | Supine | Highest | Increased episcleral venous pressure, reduced gravity-assisted outflow. (10) |
Table 1: Table showing the physiological explanation of relative IOP due to posture type
Activity Levels and Exercise
In terms of activity, standing and walking typically result in lower IOP compared to sitting. (6) Walking may reduce IOP even more than standing, likely due to a temporary decrease in central blood volume, improved venous return to the heart, and increased heart and breathing rates that promote aqueous humor drainage. While aerobic exercise is known to lower IOP, resistance exercise can raise it, with the effect depending on the intensity of the resistance. (6)
Conclusion
It is important to note that prolonged IOP fluctuations caused by changes in posture, even if IOP appears well-controlled, can contribute to the progression of visual field deterioration in Glaucoma. Therefore, giving advice on sleeping postures and daily activities is vital for optimising IOP fluctuations for Glaucoma patients. For instance, a short, brisk walk has been shown to clinically reduce IOP, with the effect lasting for over twenty minutes. (7) This unveils the importance of providing recommendations for sleeping postures and daily activities of the patient. (6) While ageing is associated with Glaucoma progression, further research is needed to fully understand its specific relationship with IOP fluctuations. (6)
References
- Machiele, R., Motlagh, M., Zeppieri, M., & Patel, B. C. (2024). Intraocular pressure. In StatPearls [Internet]. StatPearls Publishing.
- Carini, F., Mazzola, M., Fici, C., Palmeri, S., Messina, M., Damiani, P., & Tomasello, G. (2017). Posture and posturology, anatomical and physiological profiles: overview and current state of art. Acta Bio Medica: Atenei Parmensis, 88(1), 11.
- Liang, X., Wei, S., Li, S. M., Zhao, S., Zhang, Y., & Wang, N. (2024). The impact of different postures on acute intraocular pressure and accommodation responses during reading. BMC ophthalmology, 24(1), 405.
- Nelson, E. S., Myers Jr, J. G., Lewandowski, B. E., Ethier, C. R., & Samuels, B. C. (2020). Acute effects of posture on intraocular pressure. PLoS One, 15(2), e0226915.
- Ireka, O. J., Ogbonnaya, C. E., Arinze, O. C., Ogbu, N., & Chuka-Okosa, C. M. (2021). Comparing posture induced intraocular pressure variations in normal subjects and glaucoma patients. International Journal of Ophthalmology, 14(3), 399.
- Sang, Q., Xin, C., Yang, D., Mu, D., & Wang, N. (2024). Effect of different postures on intraocular pressure in open-angle glaucoma. Ophthalmology and Therapy, 13(1), 149-160.
- Hamilton-Maxwell, K. E., & Feeney, L. (2012). Walking for a short distance at a brisk pace reduces intraocular pressure by a clinically significant amount. Journal of glaucoma, 21(6), 421-425.
- Sang, Q., Xin, C., Yang, D., Mu, D., & Wang, N. (2024). Effect of different postures on intraocular pressure in open-angle glaucoma. Ophthalmology and Therapy, 13(1), 149-160.
- Sang, Q., Xin, C., Yang, D., Mu, D., & Wang, N. (2024). Effect of different postures on intraocular pressure in open-angle glaucoma. Ophthalmology and Therapy, 13(1), 149-160.
- Md Akbar, Gaurav Kapoor, Vijay Kumar Sharma, Vikas Ambiya, Srujana D, Srishti Khullar, Sushil Kumar, & Rahul. (2025). The Postural changes in intraocular pressure in normal and glaucomatous eyes in Indian population. International Journal of Health and Clinical Research, 7(4), 25–28.

Recent Comments